The Efficacy of Bee Venom Acupuncture Therapy for Bell's Palsy in the Recovery Period with Sleep Disorders: A Randomized Controlled Trial
##plugins.themes.bootstrap3.article.main##
Abstract
Background: More than one-third of patients with moderate to severe Bell's palsy (BP) have residual sequelae of varying degrees. Failure or incomplete recovery of facial nerve function will bring huge social and psychological pressure to patients, seriously affecting social activities and quality of life. Bee venom acupuncture (BVA) therapy is a rapidly developing treatment method and is widely used for patients with BP in East Asia. However, its therapeutic effect on BP during the recovery period accompanied by sleep disorders remains unclear. The feasibility of this innovative method is the focus of this study.
Objective: To explore the clinical efficacy of BVA therapy in BP complicated with sleep disorders during the recovery period.
Method: We conducted a randomized controlled trial. Patients with BP accompanied by sleep disorders were recruited and randomly divided into control group and BVA group at a ratio of 1:1. The control group received conventional acupuncture, while BVA group was treated with bee needle therapy. Both groups were provided with three treatments per week for a total of 4 weeks. The primary outcome measure was the change in the House-Brackmann Facial Paralysis Scale (HB) from baseline to week 8. The secondary outcome measures were the changes in Facial Disability Index (FDI), Pittsburgh Sleep Quality Index(PSQI), Hamilton Anxiety Scale (HAMA), and Hamilton Depression Scale (HAMD) at weeks 4 and 8.
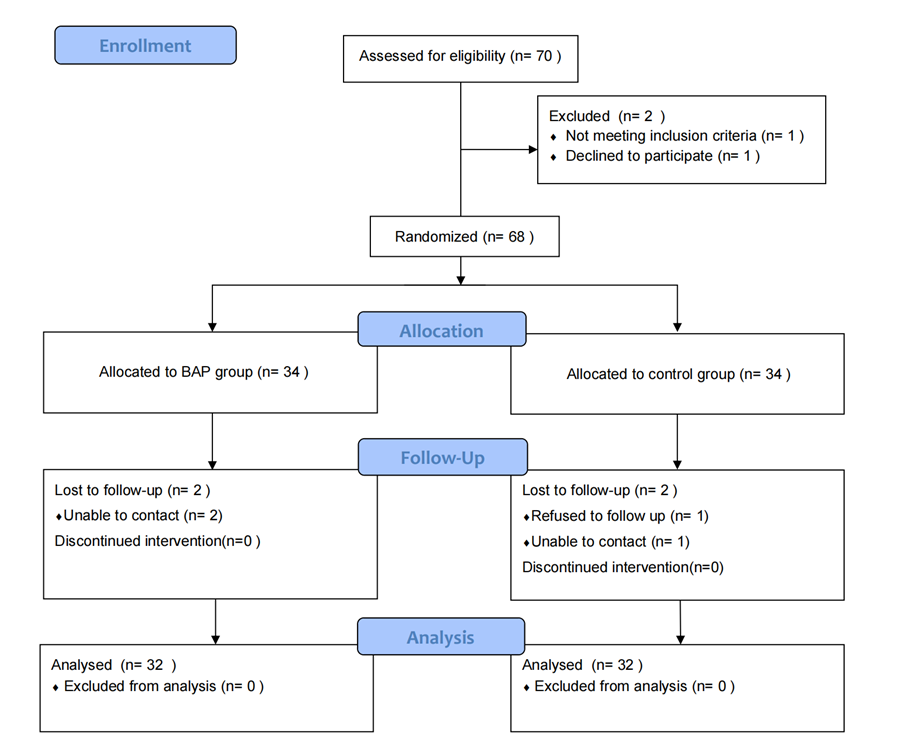
Result: Of the 70 participants enrolled, 64 (91.4%) completed the intervention and were included in the analysis. In the 8th week, the HB score of BVA group was 2.0 (0.5), which was 2.2 scores lower than the baseline ([95% CI, -2.8 to -1.6]; P<0.001). The HB score of the control group was 2.8 (0.7) scores, with an average decrease of 1.5 scores ([95% CI, -2.3 to -0.7]; P<0.001). There was a statistically significant difference between groups (P=0.002). In addition, compared with the control group, the scores of PSQI, HAMA and HAMD in BVA group were significantly decreased (P<0.05) , and the FDI score was significantly increased (P<0.05) at weeks 4 and 8. No severe adverse event occurred in either group.
Conclusion: BVA therapy is beneficial for improving the facial nerve function, sleep quality and anxiety and depression symptoms of BP patients during the recovery period, and its therapeutic effect can last for up to 4 weeks.