Global Trends and Health Inequalities in Non-Rheumatic Heart Disease Burden, 1990–2021: A Systematic Analysis of the Global Burden of Disease 2021
##plugins.themes.bootstrap3.article.main##
Abstract
Objective: To comprehensively analyze global epidemiological trends, health disparities, and future projections of non-rheumatic valvular heart disease (NRVHD), including calcific aortic valve disease (CAVD) and degenerative mitral valve disease (DMVD), from 1990 to 2021, and to forecast disease burden through 2052.
Methods: Using data from the Global Burden of Disease (GBD) 2021, we extracted estimates and 95% uncertainty intervals (UI) for incidence, prevalence, deaths, and disability-adjusted life years (DALYs) of NRVHD (including CAVD and DMVD) from 1990 to 2021. We analyzed epidemiological trends at global, regional, and national levels, assessed health inequalities, and employed Bayesian modeling to project future disease burden through 2052.
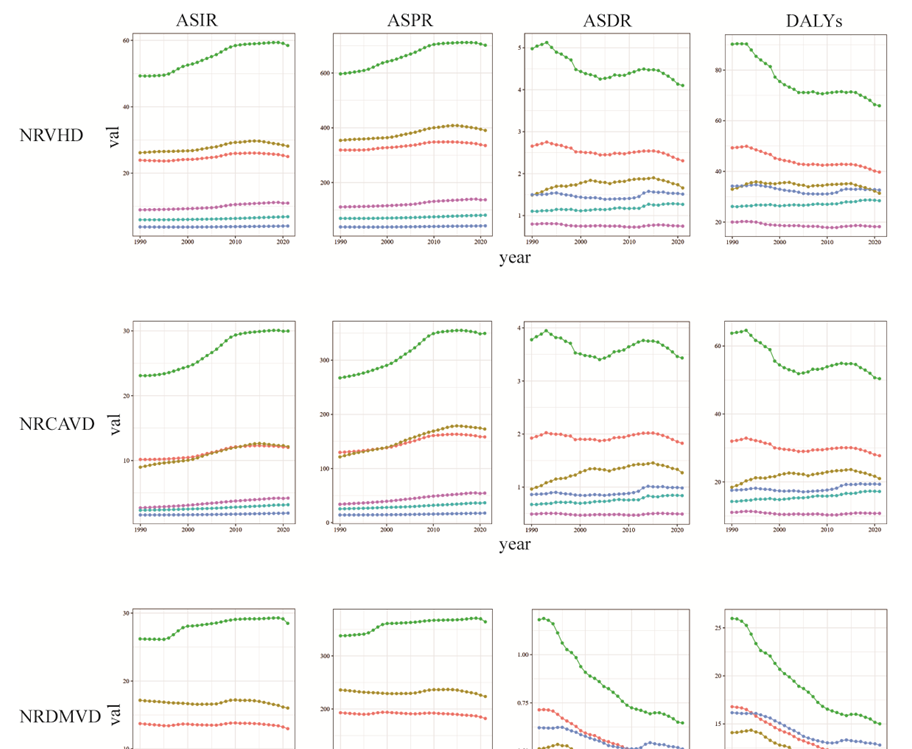
Results: In 2021, an estimated 2,206,928 global incident cases of non-rheumatic valvular heart disease (NRVHD) were recorded (95% UI: 2,048,267–2,375,325), with calcific aortic valve disease (CAVD) and degenerative mitral valve disease (DMVD) accounting for 47.32% and 52.68% of cases, respectively. Prevalence reached 28,389,034 cases (95% UI: 26,323,458–30,585,670), of which CAVD and DMVD comprised 46.92% and 54.58%. Disability-adjusted life years (DALYs) attributable to NRVHD totaled 3,238,185 (95% UI: 2,934,104–3,594,474), with CAVD contributing 69.27% and DMVD 29.13%. The burden was disproportionately concentrated in high sociodemographic index (SDI) regions, such as high-income North America, whereas low SDI regions, including sub-Saharan Africa, exhibited the lowest burden. Health inequalities widened between 1990 and 2021, evidenced by a rise in absolute disparities (the slope index of inequality increased from 99.35 to 135.92). Decomposition analysis identified population growth (55.95%) and aging (52.73%) as primary drivers of the increase in DALYs. Projections suggest a 24–26% decline in age-standardized incidence, prevalence, mortality, and DALY rates by 2052.
Conclusion: The escalating burden of NRVHD reflects demographic shifts and persistent health inequities, with high-SDI regions bearing the greatest burden. Despite projected declines in age-standardized rates, absolute case numbers will rise due to population aging. Targeted interventions—emphasizing early diagnosis, equitable resource allocation, and management of modifiable risk factors—are critical to mitigate disparities, particularly in aging high-income populations.