Anti-Neutrophil Cytoplasmic Antibody (ANCA)-Associated Vasculitis Involving the Central Nervous System with MOG-Igg Associated Disease: A Rare Case Report and Review of the Literature
##plugins.themes.bootstrap3.article.main##
Abstract
Abstract Anti-neutrophil cytoplasmic antibody (ANCA)-associated vasculitis (AAV) and Anti-myelin oligodendrocyte glycoprotein immunoglobulin G antibody (MOG-IgG)-associated disorders (MOGAD) – though both immune disorders – have rarely been reported together. Here we present their first documented co-occurrence and review CNS manifestations in AAV.
Methods We report a rare case of a 76-year-old female patient who developed MOGAD following her diagnosis of AAV. A literature search was conducted in the PubMed to analyze AAV’s clinical features in the CNS.
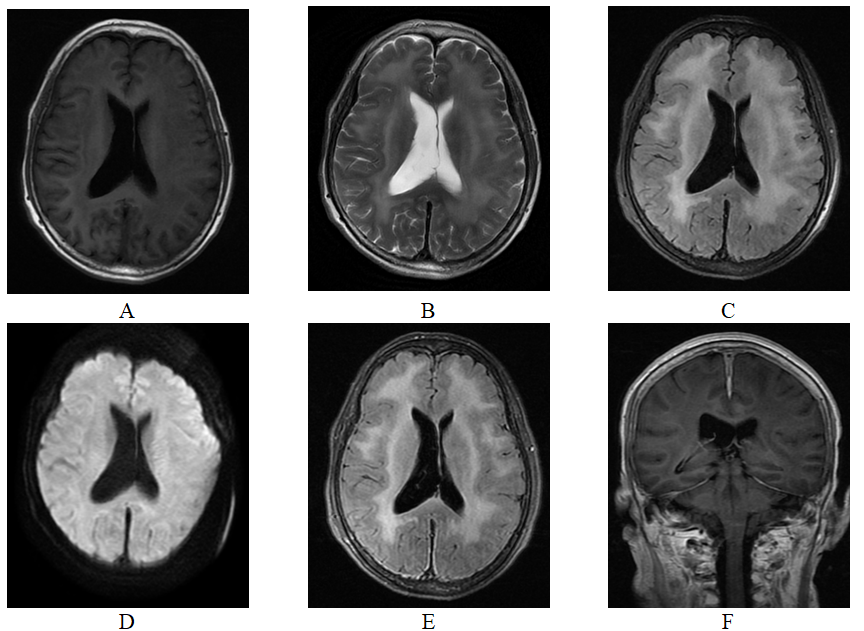
Results The patient was diagnosed with AAV after initial interstitial pneumonia and peripheral nerve injury, followed by intermittent headache, extensive abnormal white matter signals with meningeal enhancement, positive serum MOG antibody. Immunotherapy failed to relieve headache effectively, and the patient died of pneumonia after 14 months. Through a literature search, a total of 358 cases of AAV and CNS involvement were identified. The retrieved studies revealed that 102 patients had meningeal involvement, which is the most commonly affected site in the CNS. Hypertrophic pachymeningitis and ischemic stroke are the main manifestations of AAV in the CNS.
Conclusion Rare AAV complicated by MOGAD case has poor outcomes. Studies indicate AAV frequently affects the CNS via hypertrophic pachymeningitis or ischemic stroke, typically presenting with headache and dural involvement.